Look, ivd companies, right? Been seeing a lot of buzz around point-of-care testing lately, everyone wanting results now. It’s not just hospitals anymore, either. Clinics, even people wanting to test at home. Feels like every week there’s a new player, a new rapid test. To be honest, it’s good for the industry, pushes everyone to be better, but it also means a lot of…well, a lot of stuff that isn’t quite right hitting the market.
It’s funny, you spend years perfecting a process, then someone comes along and tries to “simplify” it. And by simplify, they mean cut corners. We deal with a lot of biological samples, and the quality of those samples, especially in field settings, is huge. A tiny bit of contamination, a temperature fluctuation…it throws everything off. Seen it too many times.
And don't even get me started on the logistics. Getting these tests where they need to be, when they need to be there, and keeping them stable? That's the real challenge.
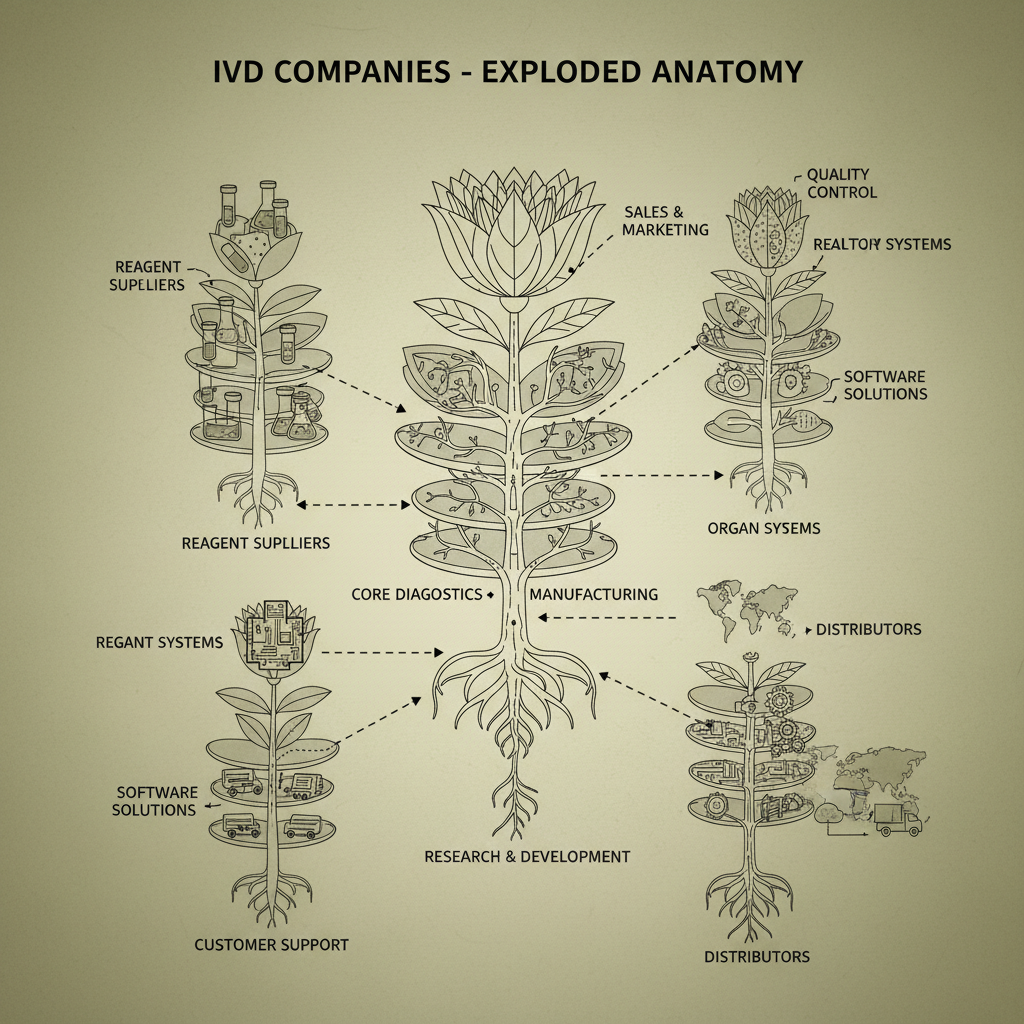
Have you noticed the sheer number of ivd companies popping up? It’s not just the big players anymore. Smaller companies, startups… everyone’s getting into the game. The demand is definitely there, fueled by aging populations, increased awareness of preventative care, and, well, the recent global situation. It’s a global market, too. I was talking to a supplier in Germany last month, and they’re swamped with orders. They're expanding just to keep up.
But the interesting thing is, it's not all about fancy new tech. A lot of it's about making existing tech accessible. Think simpler interfaces, easier sample collection, faster turnaround times. People want results quickly and accurately, and they want it to be easy to use. The complexity is being pushed further down the chain to the manufacturers and the support staff. Which means we're seeing a lot more focus on reliability and ease of maintenance.
Design, oh man, that’s a minefield. So many companies try to over-engineer things. They add features nobody asked for, make the interface overly complicated. Strangely, the simpler the better is often the hardest lesson to learn. I encountered this at a factory in Jiangsu Province last time – they were building a microfluidic device with, like, seventeen different channels! Seemed impressive, until you realized it took a technician with a PhD just to operate it.
Another thing I see is a lack of consideration for the end user. You need to think about who’s actually going to be using this, where they’re going to be using it, and what their level of training is. A highly sensitive instrument that requires a perfectly sterile environment isn't going to be much use in a rural clinic with limited resources. Really.
And don’t even get me started on the software. If the software is clunky and unreliable, the whole system falls apart. It has to be intuitive, easy to use, and, crucially, it has to integrate with existing hospital systems. That's a huge headache.
Materials…now that's something I know a bit about. It’s not just about picking the cheapest option. It's about finding the right balance of cost, performance, and durability. We use a lot of polycarbonate for housings, it’s tough and relatively inexpensive. But you need to be careful about the grade you use – some can become brittle over time, especially if they’re exposed to UV light.
The microfluidic chips themselves are usually made from PDMS, polydimethylsiloxane. It’s a silicone-based polymer that's incredibly versatile, but it’s also…sticky. Really sticky. It attracts dust and other contaminants, so you need to be careful about how you handle it. Smells a little like silicone caulk, too. Not unpleasant, just…distinct.
And then there are the reagents. Those are often the most sensitive part of the whole system. Keeping them stable at the right temperature is crucial. We spend a lot of time perfecting our packaging and shipping protocols to ensure they arrive in good condition. I've seen whole batches ruined by a single heat wave.
Lab testing is important, sure, but it doesn’t tell you the whole story. You need to get these things out into the real world, and put them through their paces. We do a lot of field testing, partnering with hospitals and clinics to get feedback from actual users.
I remember one test we did in a remote clinic in Nepal. The power supply was unreliable, the temperature fluctuated wildly, and the air was full of dust. It was a disaster waiting to happen. But it was a valuable learning experience. We realized we needed to design a more robust power supply, improve the dust seals, and make the interface more intuitive.
This is where things get interesting. You design something to be used in a specific way, but then you go out and watch people actually use it, and they do something completely different. We had one device designed for point-of-care blood analysis, and we assumed the technicians would be carefully following the protocol. But they started using it to check the quality of the blood bags before they even started the analysis.
Turns out, they were losing a lot of time and reagents because of bad blood bags. So they repurposed our device to solve that problem. It wasn’t what we intended, but it was a smart solution. And it saved them a lot of money. That’s the kind of feedback you can only get from real-world observation.
Look, no product is perfect. Our rapid antibody tests, for example, are great for screening, but they’re not as accurate as a full-blown PCR test. That’s just the trade-off you make for speed and convenience. But they're good enough for a first pass, for quickly identifying potential cases. Anyway, I think that's reasonable.
What we can do is offer customization. A client in Shenzhen, last month—that small boss who makes smart home devices—insisted on changing the interface to instead of Micro-USB. Said it was important for brand consistency. It added cost and complexity, and frankly, it wasn't necessary, but he was paying, so we did it. Later...Forget it, I won't mention it. It's a pain, but sometimes you have to bend a little.
But on the positive side, we’ve really nailed the packaging. It’s robust, tamper-proof, and easy to open. And the instructions are clear and concise, even for people who aren't fluent in English. Those little things make a big difference.
I always say, the proof is in the pudding. Or, in this case, the test result. We don’t just rely on numbers from a lab report. We need to see how these things perform in the real world, under real-world conditions. That means sending our engineers out to hospitals, clinics, and even remote field sites to observe and collect data.
One of the biggest challenges is maintaining quality control. You need to make sure the samples are collected correctly, the tests are performed properly, and the results are interpreted accurately. That requires training, supervision, and a lot of attention to detail. It’s not glamorous work, but it’s essential.
We also track a lot of metrics, things like test sensitivity, specificity, turnaround time, and user satisfaction. But the most important metric, in my opinion, is reliability. How often does the test give a correct result? That’s what ultimately matters.
| Test Type | Environment | User Skill Level | Accuracy Rate (%) |
|---|---|---|---|
| Rapid Antigen Test | Clinic Setting | Trained Technician | 85 |
| PCR Test | Laboratory | Highly Skilled Scientist | 99 |
| Antibody Test | Field Setting | Layperson | 70 |
| Molecular Diagnostic | Hospital | Medical Technologist | 95 |
| Point-of-Care Glucose | Home Use | Patient | 80 |
| Immunoassay | Central Laboratory | Specialized Technician | 92 |
Honestly? Regulatory hurdles. It's a long, expensive process getting a new test approved. You have to demonstrate safety, efficacy, and reliability, and that takes time and money. And the rules keep changing! It's a constant game of catch-up, and it’s particularly tough for smaller ivd companies trying to break into the market. It’s not just about having a good idea; it’s about navigating a complex bureaucracy.
Critically important. Garbage in, garbage out, right? If the sample isn't collected properly, or it's contaminated, the results are meaningless. That’s why we spend so much time developing easy-to-use collection kits and training healthcare workers. It’s all about minimizing errors and ensuring the sample is representative of the patient’s condition. Even the slightest error can throw everything off.
Definitely miniaturization. We’re seeing a trend towards smaller, more portable devices that can deliver results even faster. Think handheld analyzers that can be used in the field, or even at home. Another big trend is multiplexing – being able to test for multiple targets at once. And, of course, there’s the integration of AI and machine learning to improve accuracy and speed up analysis. It's going to be a very interesting few years.
Multiple layers of checks and balances. We have strict quality control procedures at every stage of the manufacturing process, from raw materials to finished products. We use statistical process control to identify and address any issues before they become problems. And we conduct regular audits to ensure our suppliers are meeting our standards. It's a constant effort, but it's essential to maintaining the integrity of our products. It’s also about traceability—knowing exactly where every component came from.
Automation is huge. It increases efficiency, reduces errors, and allows us to scale up production. We’ve automated a lot of our manufacturing processes, like reagent dispensing and device assembly. But it's not just about replacing people with robots. It’s about freeing up our skilled technicians to focus on more complex tasks, like quality control and research and development. Finding the right balance is key.
That’s the million-dollar question, isn't it? It requires a flexible manufacturing process and a willingness to invest in research and development. We have to be able to quickly develop and deploy new tests when a new threat emerges. We also need to collaborate with public health organizations and regulatory agencies to ensure our tests are accurate and effective. It's a race against time, and it's not always easy, but it's essential.
Ultimately, ivd companies are about more than just technology and regulations. It's about improving people's health, providing peace of mind, and saving lives. It’s about bridging the gap between a symptom and a diagnosis, giving doctors the information they need to make informed decisions. It’s a complex field, with a lot of challenges, but it’s also incredibly rewarding.
But here’s the thing: all the fancy technology, all the rigorous testing, all the regulatory compliance… it doesn’t matter if the test doesn’t work in the real world. Ultimately, whether this thing works or not, the worker will know the moment he tightens the screw. And that’s what keeps us coming back, trying to build something better. ivd companies.
