In vivo diagnostics represent a pivotal advancement in modern medicine, offering real-time analysis within the living organism. This capability is transforming disease detection, monitoring, and personalized treatment strategies across a spectrum of medical fields. The increasing global burden of infectious diseases and chronic illnesses demands rapid, accurate, and accessible diagnostic tools, making in vivo diagnostic technologies increasingly crucial.
The development and implementation of in vivo diagnostic methods are driven by innovations in areas like molecular biology, nanotechnology, and imaging techniques. These advancements are not only enhancing diagnostic accuracy but also enabling minimally invasive procedures and improved patient outcomes. The global market for in vivo diagnostics is experiencing substantial growth, fueled by rising healthcare expenditure and the need for proactive disease management.
Ultimately, in vivo diagnostic solutions contribute to more effective healthcare delivery by allowing for earlier interventions, reduced healthcare costs, and improved quality of life for patients worldwide. Continued research and development in this area promise even more sophisticated and personalized diagnostic approaches in the future, shaping the landscape of healthcare for years to come.
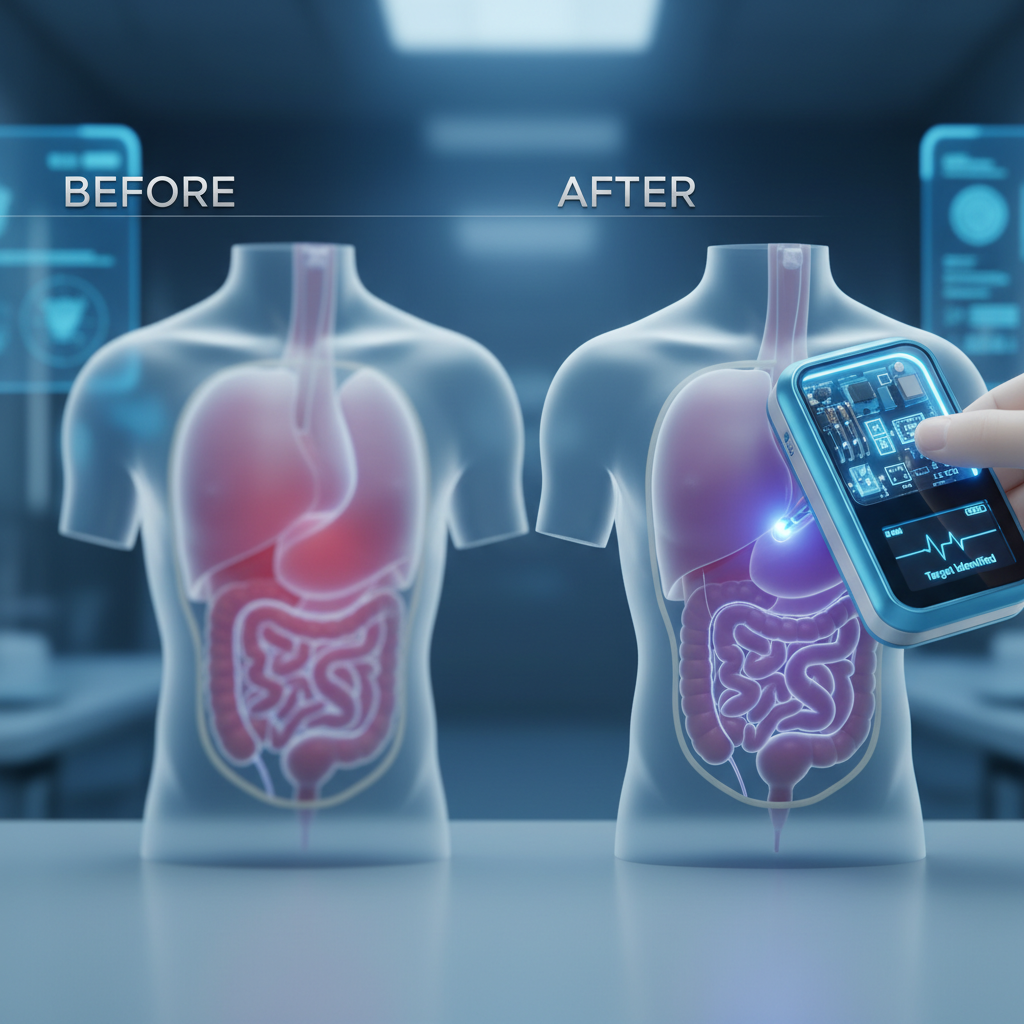
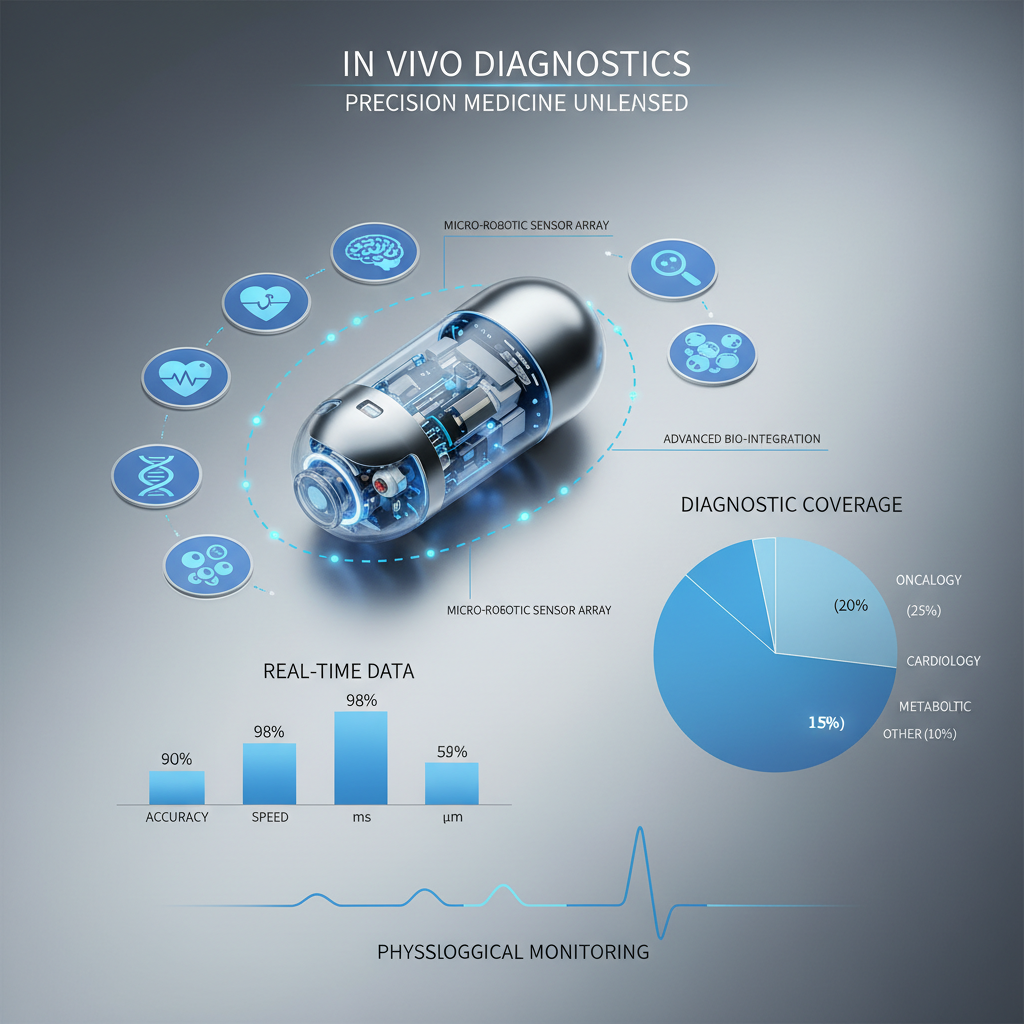
The growing importance of in vivo diagnostic stems from its ability to provide immediate, contextualized information about a patient’s health status directly within their body. This contrasts with traditional methods that often require sample extraction and laboratory analysis, leading to delays in diagnosis and treatment. The ability to see real-time responses to stimuli or disease progression is invaluable for personalized medicine.
Furthermore, the sophistication of in vivo diagnostic tools is continuously increasing, incorporating advanced imaging technologies, biosensors, and molecular probes. These tools are not only improving accuracy but also expanding the range of conditions that can be assessed, leading to earlier detection and more effective interventions.
In vivo diagnostic refers to the process of examining the internal state of a living organism without removing tissue or fluids for external analysis. This encompasses a wide range of techniques, including endoscopic procedures, medical imaging (MRI, CT scans, PET scans), and the use of implanted biosensors. The core principle is to obtain diagnostic information directly within the biological environment.
This approach is integral to modern healthcare, allowing clinicians to diagnose conditions such as cancers, cardiovascular diseases, and infectious diseases with greater precision. The ability to perform in vivo diagnostics often reduces the need for invasive biopsies, minimizes patient discomfort, and accelerates the diagnostic process.
In the context of the pharmaceutical industry, in vivo diagnostics play a critical role in drug development, monitoring drug efficacy, and personalizing treatment regimens based on individual patient responses. This shift toward personalized medicine is fundamentally changing the way healthcare is delivered, and in vivo diagnostics are at the forefront of this transformation.
The effectiveness of in vivo diagnostic systems relies on several core components working in synergy. Firstly, advanced imaging technologies are crucial for visualizing internal structures and identifying abnormalities. This includes techniques such as high-resolution endoscopy, contrast-enhanced imaging, and molecular imaging. Secondly, biocompatible sensors and probes are essential for detecting specific biomarkers or physiological changes within the body.
Data acquisition and processing are equally important. Sophisticated algorithms and software are required to analyze the data generated by these sensors and imaging techniques, converting raw data into clinically relevant information. Finally, user-friendly interfaces and data visualization tools are necessary to allow clinicians to interpret the results accurately and make informed decisions.
Furthermore, the accuracy, sensitivity, and specificity of in vivo diagnostic tools are paramount. Rigorous quality control measures and adherence to regulatory standards are vital to ensure reliable and consistent results. This encompasses calibration of sensors, validation of imaging protocols, and ongoing monitoring of system performance.
In vivo diagnostic tools are transforming healthcare globally, impacting areas ranging from early disease detection to personalized treatment strategies. In developed nations, in vivo diagnostics are widely used for cancer screening, cardiovascular disease management, and neurological disorder assessment. For instance, endoscopic procedures are routinely employed for colon cancer screening, while cardiac MRI helps diagnose heart conditions with high accuracy.
However, the impact is even more significant in resource-limited settings. Portable ultrasound devices and point-of-care in vivo diagnostic tools are enabling healthcare professionals to diagnose conditions like malaria, tuberculosis, and HIV in remote areas with limited access to traditional laboratory facilities. This is crucial for improving healthcare access and reducing mortality rates in underserved populations.
The advantages of in vivo diagnostic are numerous. Firstly, they offer a significant reduction in patient discomfort and invasiveness compared to traditional biopsy methods. Secondly, the real-time data provided accelerates the diagnostic process, enabling quicker treatment initiation. This speed is critical in conditions like stroke or sepsis where timely intervention is crucial.
The long-term value extends beyond immediate clinical benefits. Reduced reliance on invasive procedures translates to lower healthcare costs. The ability to monitor disease progression non-invasively allows for more proactive and personalized treatment strategies, potentially improving patient outcomes and quality of life.
The future of in vivo diagnostic is poised for significant innovation. Nanotechnology is playing an increasingly important role, with the development of nanoscale sensors and imaging agents that can detect biomarkers at incredibly low concentrations. Artificial intelligence (AI) and machine learning are being integrated into diagnostic algorithms to enhance accuracy and automate image analysis.
Furthermore, advancements in microfluidics and lab-on-a-chip technologies are enabling the development of portable and point-of-care in vivo diagnostic devices. These devices hold the potential to revolutionize healthcare access in remote areas and resource-limited settings. The convergence of these technologies promises a future where diagnostics are faster, more accurate, and more accessible than ever before.
Finally, the rise of wearable sensors and remote patient monitoring systems is extending the reach of in vivo diagnostics beyond the confines of the hospital, enabling continuous monitoring of patient health and early detection of potential problems.
Despite the immense potential, the widespread implementation of in vivo diagnostic faces several challenges. One key obstacle is the cost of advanced imaging technologies and specialized equipment. This can limit access to these tools in resource-limited settings. Another challenge is the need for highly trained personnel to operate and interpret the results from these complex systems.
However, innovative solutions are emerging to address these challenges. The development of more affordable and portable diagnostic devices is lowering the cost barrier. Telemedicine and remote training programs are expanding access to expertise. Furthermore, the integration of AI and machine learning is automating aspects of image analysis, reducing the reliance on specialized expertise.
Addressing data privacy and security concerns is also crucial. Robust data encryption and secure data storage protocols are essential to protect patient information and maintain trust.
| Challenge | Impact on in vivo diagnostic | Proposed Solution | Expected Outcome |
|---|---|---|---|
| High Equipment Costs | Limits accessibility, especially in low-resource settings. | Development of portable, low-cost devices. | Increased access and affordability. |
| Lack of Trained Personnel | Incorrect operation and interpretation of results. | Telemedicine training programs and AI assistance. | Improved skill level and reduced errors. |
| Data Security Concerns | Patient privacy breaches and data misuse. | Robust data encryption and secure storage. | Enhanced data protection and patient trust. |
| Regulatory Hurdles | Slows down the approval and adoption of new technologies. | Streamlined regulatory pathways for innovative diagnostics. | Faster access to new and improved technologies. |
| Integration Challenges | Difficulty integrating in vivo diagnostics with existing healthcare systems. | Standardized data formats and interoperable systems. | Seamless data exchange and improved workflow efficiency. |
| Biomarker Validation | Difficulty in identifying and validating reliable biomarkers. | Multi-center studies and data sharing initiatives. | Identification of robust and clinically relevant biomarkers. |
In vivo diagnostic offers several key advantages over traditional lab tests, including reduced invasiveness, real-time results, and the ability to assess conditions directly within the biological environment. This leads to faster diagnosis, personalized treatment, and improved patient outcomes, minimizing the delay associated with sample collection and analysis. It also decreases the risk of complications related to invasive procedures.
The accuracy of in vivo diagnostic techniques varies depending on the specific method employed and the condition being assessed. Generally, these techniques offer high accuracy, but factors like image resolution, sensor sensitivity, and operator expertise can influence reliability. Regular calibration, rigorous quality control measures, and standardized protocols are essential to ensure consistent and accurate results.
The cost of in vivo diagnostic procedures can vary significantly depending on the complexity of the technique, the facility where it is performed, and the geographic location. Advanced imaging techniques like MRI or PET scans tend to be more expensive than simpler procedures like ultrasound. However, the long-term benefits, such as reduced need for invasive procedures and improved treatment outcomes, can offset these initial costs.
While generally considered safe, in vivo diagnostic procedures can carry some risks, depending on the specific technique used. These risks may include allergic reactions to contrast agents, radiation exposure from imaging techniques, or minor discomfort during endoscopic procedures. Healthcare professionals carefully weigh the benefits and risks before recommending any in vivo diagnostic procedure and take steps to minimize potential complications.
Protecting patient data is paramount. Healthcare facilities employ robust data security measures, including encryption, access controls, and compliance with privacy regulations like HIPAA. Patient consent is obtained before any data is collected, and individuals have the right to access and control their personal health information. Secure data storage and transmission protocols are essential to maintain confidentiality.
The future of in vivo diagnostic is incredibly promising. We can expect to see further integration of nanotechnology, artificial intelligence, and microfluidics, leading to more sensitive, accurate, and portable diagnostic devices. The development of personalized biomarkers and the use of wearable sensors for continuous monitoring will revolutionize disease detection and management, paving the way for truly proactive healthcare.
In conclusion, in vivo diagnostic represents a paradigm shift in modern healthcare, offering a powerful suite of tools for early disease detection, personalized treatment, and improved patient outcomes. From its reliance on advanced imaging to its potential for integration with AI and nanotechnology, this field is poised for continued innovation. By understanding the core principles, applications, and future trends of in vivo diagnostic, we can unlock its full potential to transform healthcare globally.
Looking ahead, continued investment in research and development, coupled with strategic partnerships between academia, industry, and healthcare providers, is essential to overcome the existing challenges and accelerate the adoption of in vivo diagnostic technologies. Embracing these advancements will not only improve the quality of life for individuals but also contribute to a more efficient and sustainable healthcare system for the future.
